Lumbar Discectomy
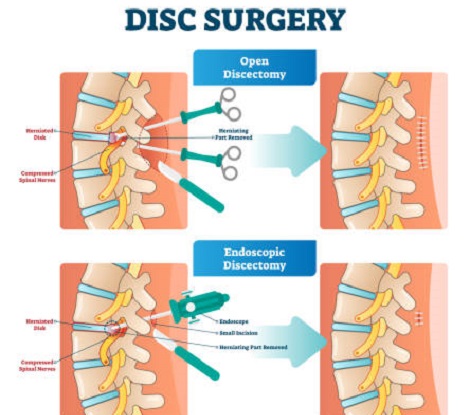
Lumbar discectomy, part of a disc in the lower back is removed to relieve pressure on spinal nerves. In particular, this procedure is extremely effective for treating leg pain (or sciatica), which is caused by a herniated disc pressing against a nerve.
As part of the procedure, the patient is generally spinally anesthetized while under sterile conditions in the operating room. The patient lies face down. The affected disc will be incised in the lumbar region by the surgeon. The herniated disc may be exposed by removing small portions of bone and ligaments. Using a surgical microscope, your surgeon examines the discs and the nerve roots.
After the procedure is complete, an antibiotic solution is irrigated into the surgical wound and closed.
What Conditions Lumbar Decompression Surgery Treat?
- spinal stenosis
- a slipped disc and sciatica
- spinal injuries
- metastatic spinal cord
What Happens During Lumbar Decompression Surgery?
Most often, you will need at least one of the following surgeries if lumbar decompression is recommended:
- An operation to relieve pressure on nerves by removing a section of bone from a vertebra (spinal bone)
- An endoscopic discectomy is performed to relieve nerve pressure caused by a damaged disc
- Stabilize and strengthen the spine by joining vertebrae with a section of bone
- Sometimes, these techniques are used in combination.
Decompressions of the spine often occur under general anesthesia, meaning you will be asleep and feel no pain during the procedure. Generally, the entire operation takes at least one hour; however, depending on how complex the process is, it can take much longer.
The surgical decision
An untreated herniated disc will generally heal within six months. The decision to undergo surgery depends on you, not your doctor. You should carefully examine all risks and benefits before going ahead with the discectomy surgery. After six weeks of nonsurgical treatment, only 10 percent of people with herniated discs require surgical intervention.
Who performs the procedure?
Neurosurgeons and orthopedic surgeons are both capable of performing spine surgeries. Complex spine surgery training is available to many spine surgeons. Especially if you’ve had a few spinal surgeries or are in a complex situation, ask your surgeon about their training.
What happens before surgery?
The surgeon can know everything about you from the consents and other forms you sign in the office (medications, bleeding history, allergies, vitamin requirements, and reactions to previous surgeries). Make sure you tell your doctor about all medicines you are taking (prescription, over-the-counter, and herbal supplements). It is likely that several days before surgery you will need to obtain pre-surgical tests (e.g., X-ray, electrocardiogram, chest, blood test,). Ask your doctor if you need to stop taking some medications before surgery.
Your surgeon will likely recommend continuing the medications you’re taking. Prevent surgery by stopping non-steroidal anti-inflammatory drugs (naproxen, ibuprofen, etc.) and blood thinners (seven days in advance). 1 week before and 2 weeks after surgery, stop using nicotine and drinking alcohol to prevent bleeding and complications with healing.
Recovery and prevention
Within two weeks of your surgery, schedule an appointment with your surgeon. Some patients may require physical therapy after their surgery.
Based on your general health and underlying condition, the recovery time may range from one to four weeks. After your surgery, you will experience pain at the incision site. You may not immediately feel relief from the pain you experienced during surgery. If you are prescribed physical therapy exercises, try to maintain a positive attitude.
People who work jobs that are not physically demanding can usually return to their jobs in two to four weeks. For jobs requiring heavy lifting or operating machinery, employees may need to wait eight to twelve weeks before returning to work.
Pain in the back often recurs. Here are a few ways to prevent recurrence:
- Sit, stand, move, and sleep with a good posture
- Fitness program that is suitable for your age and body type
- A work area that is ergonomic
- Lean body mass and healthy weight
- The use of relaxation techniques (e.g. stress management)
- Prevent smoking
What are the results?
It has been reported that patients who undergo lumbar discectomy achieve good results eighty to ninety percent of the time. An experiment comparing the surgical and nonsurgical treatment of herniated discs found the following results:
Surgery is more advantageous to people with leg pain (sciatica) than to people with back pain.
With nonsurgical treatment, less severe pain or pain that is improving is better managed.
The number of people who reported greater improvement after surgery for moderate to severe pain was significantly greater than those without.
Minimally invasive discectomy has been shown to combine the benefits of open and minimally invasive discectomy. In addition to their benefits of shorter operation times, reduced blood loss and muscle trauma, and faster recovery, minimally invasive methods are not appropriate for every patient. Micro endoscopic discectomy may be appropriate for you if you require minimally invasive surgery.
Nonsurgical treatment may not be as effective as discectomy. Surgery may make a difference later on in terms of what treatments may be needed, but this isn’t yet clear. Up to fifteen percent of patients experience an adjacent or opposite recurrence of disc herniation.
What are the risks?
There are risks associated with every surgical procedure. In addition to bleeding, infection, blood clots, and reactions to anesthesia, there are general complications associated with any surgery. Complications are more likely with spinal fusions performed concurrently with discectomies. Discectomies may cause the following complications:
An abnormal condition in which blood clots form in the veins of the legs is called deep vein thrombosis (DVT). Lung collapse or even death can occur if the clots break free and move to the lungs. DVT can be treated or prevented in several ways. Get up and out of bed as soon as possible so your blood is moving and less likely to clot. You can prevent blood pooling in your veins by wearing a support hose and pulsatile stockings. There may also be drugs used, such as Coumadin Heparin, or aspirin.
Problems with the lungs. After discectomy surgery, it is vital that the lungs provide sufficient oxygen to the tissues in order to heal. A collapsed lung can lead to pneumonia due to the buildup of mucus and bacteria. You will be encouraged by your nurse to cough often and breathe deeply.
Persistent pain or nerve damage. Nerves and the spinal cord can be damaged during any spine operation. If damaged, they could become numb or paralyzed. In most cases, nerve damage caused by the disc herniation itself is the cause of persistent pain. Decompressive surgery may not be able to heal some disc herniations permanently. Other treatment options may be available. Be realistic about what you expect from the surgery. Speak with your doctor about your expectations.
If you have above symptoms and conditions, WeCare Medical Specialty Group can help you. We have five offices across Northern Jersey. Please call our office at (973)996-2990 or book an appointment online immediately.